Passion for perfection

Periodontal Health — Recognising the Signs Early
Do your gums bleed when you brush your teeth?
Bleeding gums may indicate gingivitis, an early and reversible stage of gum inflammation, which, if left untreated, can progress to periodontitis. Periodontitis is a more advanced condition that can affect the supporting structures of the teeth and is associated with broader systemic health considerations, including cardiovascular and respiratory conditions, as well as tooth loss.
How Does Gum Disease Develop?
The Development of Gum Disease
Plaque is simply a yellowish-white film composed of bacteria, small particles, proteins and mucus. This plaque continuously accumulates on the teeth and gums.
With proper brushing and flossing, plaque is easily removed. If plaque is not removed by brushing and flossing, over time, plaque will calcify (harden).
This hardened plaque is known as tartar and can no longer be removed with simple brushing and flossing, it must be removed through our professional dental cleaning.
The more harmful bacteria release toxins which damage the gums. They also cause infection and inflammation which activates the immune system. This inflammation of the gums is called is called gingivitis and is the first stage of gum disease.

Clinical Advantages of Biological Periodontal Treatment.
:
1. Comfortable treatment — in many cases, without injections or post-procedural numbness
2. Reduced reliance on antibiotics, supporting your microbiome and systemic health
3. Efficient treatment with reduced chair time
4. A procedure that is precise, clinically controlled, and well tolerated
5. A structured, calm clinical environment designed to replace anxiety with confidence and ease
6. The treatment is entirely autologous — using only your body’s own biological resources, with no foreign additives and no risk of allergic response
Assisted Gingivitis & Periodontitis Management
Laser treatment is an effective approach for the management of early-stage gingivitis. Through targeted laser application delivered over a structured series of sessions, we are able to reduce bacterial load and inflammatory toxins — supporting the resolution of gum inflammation with precision and minimal discomfort.
Left untreated, gingivitis may progress to periodontitis — a more advanced condition that is frequently asymptomatic. Bacterial infection affecting the supporting bone and periodontal ligaments can develop silently, without noticeable pain, making regular clinical assessment essential.
Over time, untreated periodontal disease may lead to progressive bone loss and reduced tooth stability, compromising normal function and long-term oral health.
Oral health and systemic health are closely connected. Periodontitis has been associated with systemic conditions including cardiovascular disease and diabetes — a well-documented relationship that underscores the importance of maintaining a healthy oral environment as part of overall health management.
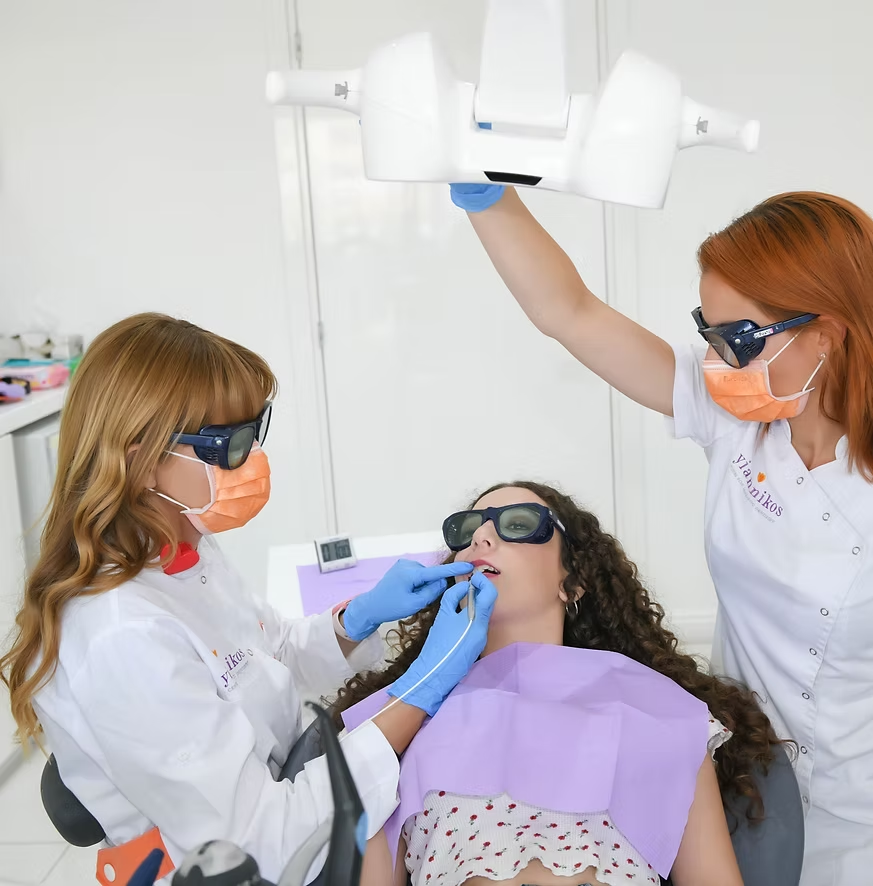
Our Periodontal Care Protocol with laser & PRF
Our periodontal care protocol combines thorough removal of plaque and deposits from root surfaces with targeted dental laser technology — reducing bacterial load and inflammatory by-products with precision and control.
This integrated approach supports the reduction of inflammation and creates the biological conditions necessary for gum healing — stabilising periodontal disease and restoring oral function over time.
We also incorporate PRF (Platelet-Rich Fibrin) — an autologous concentration of growth factors that supports tissue healing and regeneration through the body’s own natural processes, without the introduction of foreign biological material.
The oral cavity does not exist in isolation. It is an integral part of the body, and its health is inseparable from overall systemic health — a principle that guides every decision we make in periodontal care.
Frequently asked questions
What is gum disease?
Gum disease is a chronic infection affecting the gingiva and supporting periodontal structures. It develops from bacterial plaque accumulation, which can mineralize into calculus, triggering inflammation and progressive tissue breakdown.
What are the clinical signs of gum disease?
Early stages may present with minimal or no discernible symptoms. As the condition progresses, signs include gingival bleeding, inflammation, recession, tooth mobility, and persistent halitosis.
What are the causes of gum disease?
The primary cause is bacterial plaque accumulation. Additional risk factors include inadequate oral hygiene, smoking, certain medications, systemic conditions such as diabetes, and genetic predisposition.
How is gum disease treated?
Prevention remains fundamental through consistent oral hygiene and regular professional care. Treatment involves meticulous mechanical debridement of plaque and calculus from root surfaces under controlled anesthesia. Laser therapy is applied to reduce bacterial load and neutralize pathogenic toxins. PRF is introduced to support regeneration through growth factors and natural healing mechanisms. Periodontal health is directly linked to systemic conditions, including cardiovascular disease and diabetes.
What are the benefits of biological periodontal treatment?
Biological protocols using laser and PRF ensure a minimally invasive, well-tolerated clinical experience. They reduce procedure time, eliminate the need for antibiotics, and support natural healing without additives or adverse reactions.
How harmful is gingivitis?
If left untreated, gingivitis can progress to periodontitis, leading to irreversible damage of supporting structures. This progression involves bacterial infection of bone and periodontal ligaments, resulting in bone loss and gradual tooth mobility, often without pain.
How can gum disease be prevented?
Effective prevention requires disciplined oral hygiene, including brushing twice daily for two minutes and daily flossing. Regular professional examinations and cleanings are essential to maintaining periodontal stability and enduring oral health.
Can gum disease contribute to systemic health conditions?
Yes. Periodontal disease is associated with increased risk of cardiovascular conditions, including heart disease and stroke. It is also linked to pregnancy complications and may elevate susceptibility to respiratory and systemic infections.
What indicates progression of gum disease?
Recognition of worsening signs is essential for timely intervention. These include increased bleeding during brushing or flossing, advancing gingival recession, tooth mobility, and persistent halitosis.